|
AIRBORNE ALLERGIES (ATOPIC DERMATITIS)

|

|
Every one knows someone with “hay fever.” Airborne pollens, molds, dust particles, etc. are inhaled and soon the sneezing and sniffling begins. A simple way to think of atopy for pets would be simply saying that the airborne allergen is inhaled by the pet but instead of sneezing and sniffling, the pet gets itchy skin. In fact, this was what we thought was happening for many years but the situation turns out more complicated.
In atopic dermatitis, airborne pollens, molds, dust particles etc. gain entry to the skin through a defective skin barrier. Inhaling is not involved. The immune system becomes inflamed by the airborne allergens and soon the itching and scratching begins. The allergens come from the air but the itch is manifested in the skin.
|
Airborne particles (pollens, danders etc.) are harmless to someone who is not allergic to them.
Allergy develops in individuals who are genetically programmed to do so.
Breeds predisposed to develop atopy
|

Dalmatian
(Photocredit: MorgueFile.com)
|

Golden
Retriever
(Photocredit: MorgueFile.com)
|

West Highland
White Terrier
(Photocredit: MorgueFile.com)
|

Shar Pei
(original graphic by marvistavet.com)
|

Labrador
Retriever
(Photocredit: MorgueFile.com)
|
|
|
|
|
|
|
|

Cairn Terrier
(Photocredit: Kathrin Albrecht via Wikimedia Commons )
|

Lhasa Apso
(Photocredit: MorgueFile.com)
|

Shih Tzu
(Photocredit: MorgueFile.com)
|

Boxer
(Photocredit: MorgueFile.com)
|

Pug
(Photocredit: MorgueFile.com)
|
FEATURES OF ATOPY IN DOGS
There are many reasons for pets to itch: parasites, allergy to flea bites, food allergy, secondary infection and the list goes on. The following are findings in the history and examination of the patient that might lead to a diagnosis of atopy. (In fact, meeting 5 criteria from this list yields an 85% accuracy for the diagnosis of atopic dermatitis, at least for dogs:
- Young age of onset
Seasonal itchiness due to atopy tends to begin early in a pet's life (between ages 1 and 3 years in 70% of dogs diagnosed with atopy). Food allergy tends to begin later (more like age 5 or 6 years in dogs) or earlier (less than 6 months of age). Age at which itching first manifests is not as reliable a sign in cats as in dogs.
-
Mostly indoor lifestyle
It is indoors where many airborne allergens concentrated; however, it is important to note that allergens in the air are in the air for miles it is not easy to escape allergens by simply going outdoors nor by simply going indoors.
- Good response to steroids
Whether the patient is a dog or cat, itchiness due to atopy responds rapidly to cortisone-type medications (prednisone, betamethasone, dexamethasone, etc.) as does itching due to insect bite allergy. Food allergy is more variable in its response; it may or may not respond well.
-
Chronic or recurring yeast infections in the skin
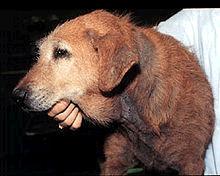
Yeast (Malassezia pachydermatis) live on the surface of the skin normally but with all the changes allergy causes to the microenvironment of the skin, yeast will proliferate and create a stinky, thickened, pigmented skin that resembles elephant skin or even tree bark. Environmental allergy is a strong predisposing factor in the development of yeast dermatitis. For more information click here.
- Front feet involved
Whether it is chewing the top of the feet or between the toes, foot licking is a classic feature of atopic dermatitis.
- Ear flaps involved
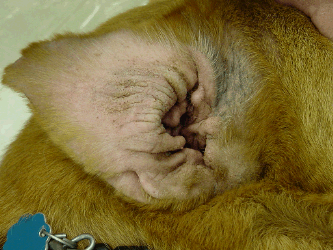
The non-haired (inside) portion of the ear flap (the "concave pinna") is commonly involved in atopic dermatitis regardless of whether the inflammation extends down the ear canal and leads to what we usually think of as ear infection. The concave pinnae become greasy, red, thickened, smelly or any combination of the above.
(Photocredit: Carol Foil via Wikimedia Commons)
- Ear margins not involved
Ear margin involvement is suggestive of sarcoptic mange and would lead one away from airborne allergies.
- Lower back area not involved
The lower back is the flea bite zone (frequently called a "California Wedge"). There are very few conditions other than flea bite allergy that cause itching in this area so if this area is involved, one must make sure flea control is achieved before further evaluating the skin.
- Seasonal Symptoms
Seasonality of the itching is also a clue towards an airborne-related allergy but since there are many climates where seasons are ambiguous, this is not necessarily a hard and fast feature of atopic dermatitis. Classically, airborne allergy symptoms are present only during certain seasons of the year or are decidedly worse during certain seasons of the year. It should also be noted that, while skin testing and blood testing are used to make immunotherapy sera for treatment of atopic dermatitis, reactions and positive results on these tests do not contribute to making a diagnosis of atopic dermatitis. Many normal animals will have positive results. These tests are for animals where the diagnosis of atopic dermatitis has already been made based on the above criteria as well as ruling out other itchy diseases.
THERE IS NO TEST FOR ATOPIC DERMATITIS
| Unlike other diseases where a test of some sort can be performed, atopic diagnosis is a "clinical diagnosis" which means the diagnosis is made based on symptoms and findings such as those listed above. "Allergy testing," which is done either by skin test (as shown on the right) or by blood testing is not a test for atopic dermatitis; instead this type of testing is done after the diagnosis has been confidently made based on findings in the patient. "Allergy testing" is conducted to determine how best to make an allergy shot serum for a specific patient; it is not part of disease diagnosis. |
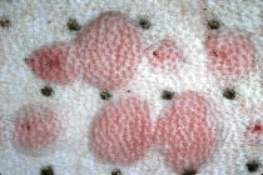
Different allergens are injected into the patient's skin
to test for reaction. The most reactive substances will
most likely be chosen for the allergy serum. Testing is
done in patients already diagnosed with atopic dermatitis. |
FEATURES OF ATOPY IN CATS
In cats, the irritation pattern is not as characteristic. There are four common manifestations of atopy:
|
Non-lesional Fur Mowing
In this situation, the cat licks away hair but seems to spare the actual skin. The area may look so precisely "mowed" that one would think someone had shaved it or it can be more haphazard. The skin is normal in appearance which is why it is called "non-lesional." Often the human family has not noticed the excessive grooming of the cat as cats are frequently very secretive about their excessive grooming. If there is any doubt as to whether the fur is falling out or being licked off, a microscopic exam of the hair will settle the question.
|
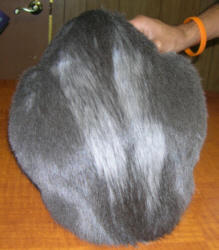
Non-lesional fur mowing(original graphic by marvistavet.com)
|
|
Eosinophilc Granuloma
This is a more extreme version of allergy where the allergic inflammation is so damaging to the skin cells the the cellular contents are released to create even further inflammation. These lesions can be in any of several parts of the body and are frequently red, raised plaques in the skin.
|
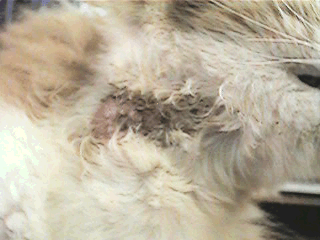
Eosinophilic Granuloma Complex
(original graphic by marvistavet.com) |
|
Miliary Dermatitis
The term "miliary" means "seed-like" and it is easy to see how this term applies to a cat with this condition: there are multiple tiny scabs covering the area of inflamed skin. This pattern of dermatitis is not specific to atopic dermatitis by any means but it is still one of the ways that atopic dermatitis can present in the cat.
|
Miliary Dermatitis (small seed-like scabs)
(Photocredit: CarolDermoid via Wikimedia Commons)
|
|
Face and Ear Itching
This is fairly self explanatory. Some cats with atopic dermatitis will manifest with self-inflicted skin irritation on their faces and around their ears.
|

Face and ear itching
|
Unfortunately, these same irritation patterns can be found in numerous other skin conditions and, in fact, up to 25% of atopic cats have multiple types of allergies.
TREATMENT OPTIONS
Many people are frustrated by the fact that treatment of atopic dermatitis focuses on controlling the symptoms. Unfortunately, finding out what a pet is allergic to is not entirely possible and even when it is, because pollens etc. circulate in the air for miles, one can't simply avoid allergens that are in the air. Only hyposensitization treatment stand a chance at actually changing the patient's immune system so that they are no longer allergic but this is far from a "sure thing." The good news is that at the end of the day, the goal is healthy comfortable skin and there is a lot that can be done towards achieving this. How big a project this becomes depends on an individual patient's ability to respond to different therapies or combinations of therapies. Here are some of the options:
|
Clearing Secondary Infections
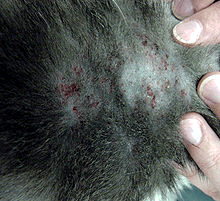
Before doing anything else, it is important to clear up secondary infections. Secondary infections involve bacteria (usually Staphylococci) and/or yeast (Malassezia) at the site of the itchiest areas on the body. These organisms live naturally in the skin but when the skin is irritated, they gain access to inner tissue layers and proliferate. Sometimes they actually come to generate further allergic response in the skin. These infections tend to be recurrent and are the usual cause of recurrence of itch symptoms in a patient previously controlled.
|
Dog with yeast dermatitis
(Photocredit: CarolDermoid via Wikimedia Commons)
|
Many patients will not be particularly itchy in between infection flare-ups so it is especially important that these be controlled. Treating flare-ups may be the only therapy needed but there will be other patients who require therapy through out their allergy season.
Hyposensitization (Allergen Specific Immunotherapy)
Hyposensitization, more commonly known as "allergy shots," is by far the treatment of choice of atopic dermatitis. All the other medications are basically just itch relief; only hyposensitization actually changes the immune system. Some dogs are eventually able to go off all treatment and are no longer allergic after they have been on hyposensitization long enough. Most dogs experience at least enough improvement to require fewer additional treatments but there are some caveats before making an appointment for allergy testing:
- Allergy shots require approximately 6-12 months to begin working.
- 25% of atopic dogs will not respond (these are usually the animals allergic to multiple allergens.)
- 25% will require prednisone or similar steroid at least at some times.
- You will most likely have to give the allergy shots yourself.
- Referral to a veterinary dermatologist will likely be necessary.
In hyposensitization the patient is injected with small amounts of allergens on a regular basis. As time passes, the amounts of allergens increase and injections are given at longer intervals. The selection of allergens is made based on the results of either an intradermal skin test (as described above), an “in vitro” test (a blood test) or a combination of the results of both tests. The younger the pet when this treatment starts, the better it works. For more details on allergen specific immunotherapy click here.)
Steroid Hormones
These cortisone-type medications (prednisone, prednisolone, triamcinolone, dexamethasone etc.) have been useful as the "first line of defense" against itchy skin for decades and they are still widely used. There are negative side effects with higher doses as well as with long term use so the trend is to use other medications to either remove the need for steroids or reduce the steroid amount needed for itch control. A higher dose is used at first but this is quickly tapered down once the condition is controlled. Prednisone, for example, is given every other day so as to allow the pet one day of recovery from the prednisone's hormonal actions. An atopic pet will usually respond within days.
Side effects include:
- Excess thirst
- Excess hunger
- Excess urination (which could lead to house-breaking issues)
- Suppression of the immune-system/bringing out latent infection (especially urinary tract infection and upper respiratory infection.)
- Raising blood sugar/destabilizing a borderline diabetic (especially a problem for cats if long-acting injectable steroids are used). In the short term, side effects can be controlled by adjusting dosage but in the long term, these medications are more problematic and if possible their use should be minimized.
Steroid hormones are very useful for acute flare-ups as well as for long term management of atopic dermatitis (assuming limits are placed on how long they are used). Side effects are greatly minimized when steroids are used topically.
Cyclosporine
Cyclosporine is a modulator of the immune response that has been very helpful in organ transplant patients both human and non-human. It has been found to be reliably effective in atopic dermatitis and does not carry the unpleasant side effect profile that steroids do. That said, it is not without side effects of its own. It is used mostly in dogs but can also be used in cats. It is for long term management and is not helpful for acute flare up control. For more details on this medication click here.
Oclacitinib
This is a new medication best used for itch relief and blocking itch symptoms. It has been especially popular as it works very fast. It does not address the inflammation in the skin; it just stops the itch sensation. This means that infection still needs to be controlled. For more details visit: www.marvistavet.com/oclacitinib-maleate.pml
Canine Atopic Dermatitis Immunotherapeutic (Cytopoint®) Injections
This is a new treatment which uses vaccine technology to eliminate one of the main mediators of itch sensation. The injections provides relief from itching for 1 month in 80% of dogs (many dogs experience relief for longer) and show effectiveness usually within 24 hours of the injection.. For many dogs, relief of itch stops the vicious cycle of itch/infection. Again, infections, if present, still need treatment but the sensation of itch is usually controlled. For more details, visit cytopoint4dogs.com.
Proper Coat Hygiene/Removing Allergens From the Environment If Possible
- Bathing the pet weekly to remove allergens from the fur may be helpful in reducing allergen exposure plus tepid water is soothing to itchy skin. There are also many therapeutic moisturizing shampoos that can be used to restore the skin’s natural barrier or to assist in general itch relief. For more details, see our section on Itch Relief.
- Avoid stuffed toys, wash bedding regularly. This minimizes dust mite exposure. Also, remove the pet from the area when vacuuming or dusting.
- Use air-conditioning and/or an air filter system.
- Keep the pet away from the lawn while it is being mowed.
- Minimize houseplants.
Omega 3 Fatty Acid Supplements
These products are NOT analogous to adding dietary oil to the pet's food, be it olive oil, coconut oil, corn oil etc. Instead, these special fatty acids act as medications, disrupting the production of inflammatory chemicals within the skin. By using these supplements, it may be possible to postpone the need for steroids/cortisones or reduce the dose of steroid needed to control symptoms. It takes a good 6 weeks to build up enough omega 3 fatty acids in the body to see a difference.
Ultra-Microsized Palmitoylethenolamide or "PEA" (Redonyl®)
PEA is a natural substance made by both plants and animals. In animals, it is involved in restoring balance to the skin's biochemistry and preventing release of the biochemical mediators of itching. (The actual process involves enhancing levels of endogenous endocannabinoids and is fairly complex.) The commercial product uses an extract of soybeans to obtain its PEA and creates a super concentrate as it would not be possible to eat enough soybeans to garner a therapeutic dose of PEA. The super small "ultra micronizing" allows for better absorption of the product. It is available as a flavored chew for dogs and can also be used in cats.
Antihistamines
Antihistamines have been popular for many years for pets, it seems their effectiveness does not stand up to scrutiny. They do not provide either short term relief nor reliable long term relief. They may be helpful in combination with other products in that their use may reduce the need for other products. They may work better in cats than in dogs.
Solid Flea Control
| Allergies are additive. This means that when a patient has multiple allergies, each allergy alone may not be enough to cause itching but the allergies all active together probably will. Consequently, taking away one of the active allergies may be enough to allergy reduction to resolve the itching. Flea bite allergy is extremely common. We now have so many effective products available that there is no reason for an animal to contend with a flea bite allergy. This simple bit of therapy (flea control) may be enough to bring the pet below his or her itch threshold without having to contend with any of the therapies listed above. |
 |
Itchy skin has been the scourge of dogs and cats for decades if not centuries. We are now armed with great understanding of immunology and have many tools to address allergy symptoms. Your veterinarian can guide you further with regard to a proper regimen or you may wish to consider seeing a veterinary dermatologist for more specialized guidance. To locate the nearest veterinary dermatologist, click here.

Page last updated: 2/9/2022
|