|
VESTIBULAR DISEASE

 Gilbert with vestibular signs Gilbert with vestibular signs
(Photocredit: Rumin8er via YouTube) |
Vestibular disease signs are frequently sudden and dramatic. The pet's head tilts to one side and the eyes dance back and forth in what looks like some kind of neurologic disaster but generally turns out not to be serious at all. Frequently a senior pet is assumed to have had some kind of stroke and is presented as an emergency or for euthanasia but, in the most common forms of vestibular disease, the pet will be back to near normal in a matter of days with no treatment. What can possibly be going on? As usual, we will begin at the beginning. |
WHAT ON EARTH IS THE VESTIBULAR APPARATUS AND HOW DOES IT WORK?
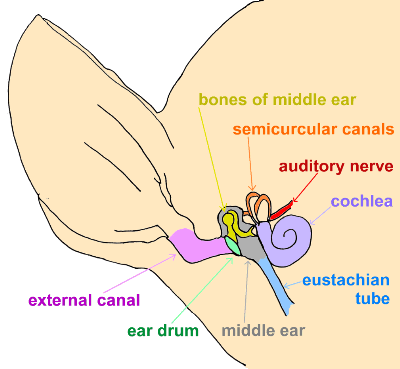
(original graphic by marvistavet.com) |
In a nutshell, the vestibular apparatus is the neurologic equipment responsible for perceiving one's body's orientation in relation to the earth (determining if you are upside-down, standing up straight, falling, rolling etc.). The vestibular apparatus and brain/cerebellum are connected and together they inform one's eyes and extremities how they should move accordingly.
The vestibular apparatus allows us to walk, even run, on uneven ground without falling, helps us know when we need to right ourselves, and allows our eyes to follow moving objects without becoming dizzy. If you think about it for a minute, it is actually pretty amazing that any of this is possible so we will take a moment to explain how it works but if you feel you pretty much have the concept, feel free to move on to the next section. The short version is that they vestibular system consists of the structures of the middle ear, the nerves that carry their messages to the brain/central nervous system, and the brain/central nervous system itself.
The vestibular system is considered to have two parts: the peripheral part (the middle ear structures and inner ear nerves) and the central part (brain and cerebellum). Vestibular disease is classified as either peripheral or central.
|
WHAT'S IN THE MIDDLE EAR?
There are two sets of receptors involved: one to detect rotational acceleration (tumbling or turning) and one to detect linear acceleration and gravity (falling and letting us know which direction is up and which is down). Both receptors are located in the middle ear.
Rotation is detected using the three semicircular canals as shown above. These canals contain fluid called endolymph, which moves as one's head rotates. Tiny neurological hair cells project into this fluid and are stimulated by the flow. These hair cells are part of sensory nerves that carry the appropriate message to the cerebellum (part of the brain that coordinates walking, running and any other locomotion) and to four vestibular nuclei in the brain stem.
These small otoliths move with gravity within a fluidy gel, stimulating small hair cells as they move similar to the situation described above.
THE SIGNS OF VESTIBULAR DISEASE
|
If there is trouble in the vestibular apparatus, then one may not properly perceive one's orientation. To put it more simply, one won't know which way is up, whether or not one is standing up straight or slanted, and one will feel very dizzy.
The following are signs of vestibular disease:
- Ataxia (lack of coordination without weakness or involuntary spasms - in other words, stumbling and staggering around).
- Motion sickness.
- Nystagmus (back and forth or rotational eye movements. The movements will be slower in one direction. This is the side where the neurologic problem is likely to be; however, nystagmus is named according to the direction of the fast component - i.e. the patient may have "left nystagmus" but the problem is probably on the right side of the vestibular apparatus).
- Circling (usually toward the side of the lesion).
- Head tilt (usually toward the side of the lesion).
- Falling to one side (usually toward the side of the lesion).
Vestibular signs are commonly (and usually incorrectly) referred to as a stroke. While a vascular accident is a possible cause of vestibular signs, it is a rare cause. Vascular disease, while common in people, is unusual in pets.
|
(Photocredit: BestBuyFromMe via Youtube.com) |
CAUSES OF VESTIBULAR DISEASE
Vestibular signs are commonly (and usually wrongly) referred to as a “stroke.” It should be noted that while a vascular accident is a possible cause of vestibular signs, it is a rare cause. Vascular disease, while common in people, is unusual in pets. In fact, there are several causes of vestibular signs:
- Inner or middle ear infection
- Hypothyroidism (the ear nerves swell and become irritated as they pass through the canals of the skull)
- Cancerous growths in the brain or involving the peripheral nerve/ear structures
- Vascular Accident (stroke)
- Toxins (heavy metals, certain medications that are toxic to the ear)
- Head injury
- Brain infection
- Congenital disease
- Parasitic (larval migration in the brain - a feline problem)
- Old dog" or "idiopathic" vestibular disease (probably the most common scenario)
Vestibular symptoms can be very disturbing to see in one's pet and there is a tendency to assume that some devastating brain event has occurred and, in fact, the most causes of vestibular symptoms at least in dogs are not serious. The most important aspect of evaluation is to determine if the problem is peripheral or central, as mentioned.
DETERMINING PERIPHERAL (EAR) VS. CENTRAL (BRAIN)
There will be some hints in the clinical presentation that the patient in question has a brain lesion causing the vestibular signs. For example, if other cranial nerves are involved and they are on the side opposite from the head tilt, then the lesion is likely to be in the cerebellum (central). If other cranial nerves are involved but they are on the same side as the head tilt, the problem could be either central or peripheral depending on which nerves are involved. If the nystagmus is vertical (the eyes are moving up and down rather than back and forth) or only exists when the animal is placed in certain positions, then the lesion is more likely to be central. Dogs with central disease tend to have altered awareness or general weakness separate from the clumsiness. The eye movements tend to be slower in central disease than they are in peripheral disease.
The external ears will be checked for infection but lack of infection in the outer ear does not necessarily indicate lack of infection in the middle ear. A clue for peripheral disease would be facial nerve paralysis where the facial expression goes lax only on the side of the head tilt. This happens because the facial nerve passes by the middle ear and frequently gets caught up in middle ear inflammation. Similar a Horner syndrome, where the pupil is small and the eye squints happens with middle ear infection as the sympathetic nerves involved get caught up in middle ear inflammation. These deficits suggest a middle ear infection is afoot even if the outer ear canals are clean.
|

Dog having a CT scan
(Photo courtesy of Justin M. Goggin, DVM,
Diplomate American College of Vet. Radiology
Vet MRI and RT Center of NJ)
|
If the vestibular signs have a clear central origin, imaging of the brain will be important in determining the nature of the lesion and what treatment makes the most sense. This means a CT scan or MRI to image the brain and most likely a referral to a specialist will be needed for this type of procedure. General anesthesia is required for CT and MRI.
If it is not clear whether the case is central or peripheral, it is prudent to wait a few days before pursuing more advanced diagnostics so as to rule out "idiopathic" vestibular disease as described below.
IDIOPATHIC DISEASE
Canine idiopathic vestibular disease (also called "Old dog vestibular disease") and, its feline counterpart, feline idiopathic vestibular disease, begin acutely and resolve acutely. Usually improvement is evident in 72 hours and ]the animal is normal in 7-14 days, possibly with an occasional head tilt persisting. When a case of vestibular disease presents, it may be a good idea to wait a few days to see if improvement occurs before doing diagnostics beyond a routine blood/urine database. These two conditions are idiopathic, meaning we do not know why they occur. We do know that they represent problems in the periphery (nerves of the middle ear rather than in the actual brain.)
Treatment of idiopathic vestibular disease generally involves control of nausea (motions sickness) while the condition runs its (relatively short) course.
IDIOPATHIC VESTIBULAR DISEASE IS THE MOST COMMON FORM
OF VESTIBULAR DISEASE IN DOGS AND CATS.
OBVIOUS EAR INFECTION?
If the patient has a history of recurrent ear infections and/or there is a facial paralysis or Horner syndrome and especially if there is debris in the outer canal, this is all pretty good evidence of middle/inner ear infection. The ear will need to be flushed out until the ear drum is visible. If the ear drum looks diseased it can be punctured and secretions released for a culture sample. At least six weeks of antibiotics will be needed for this infection. A severe infection may need a more definitive surgery such as a bulla osteotomy to drain the inner ear chambers.
STILL VESTIBULAR AFTER 3 DAYS WITH NO IMPROVEMENT? STILL NOT SURE IF IT IS THE MIDDLE EAR?
| This is where it gets a bit tricky. A CT scan or MRI will be helpful in viewing the inner ears as well as the brain and all questions can be settled. Radiographs can be taken to check the bone structures of the inner ears but radiographs turn out to be insensitive compared to newer imaging and one may end up without an answer if only radiographs are used. |
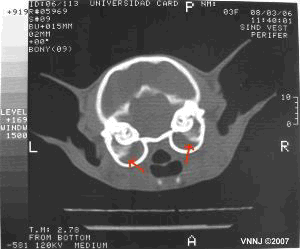
CT scan of tympanic bullae
(although this image is from a cat) |

Page last updated: 8/24/2024
|