|
Canine Leptospirosis

Leptospirosis is a challenging disease. Its symptoms are varied, as is severity, which muddies the clinical picture and complicates diagnosis. Test results can be hard to interpret, often requiring multiple samples. Tracking outbreaks is fraught with difficulty because of the cost of testing which in turn leads to under-diagnosing and under-reporting illness. Despite this, most experts feel the incidence of leptospirosis is increasing and, if all that wasn't enough, the infection is contagious to humans.
So where do we start? Let's begin where the infection begins: with the organism itself.
|
About the Organism
Leptospira organisms are spiral-shaped bacteria called spirochetes. There are several species of leptospires, but the ones that cause disease have been grouped into one particular species called Leptospira interrogans sensu lato.
|
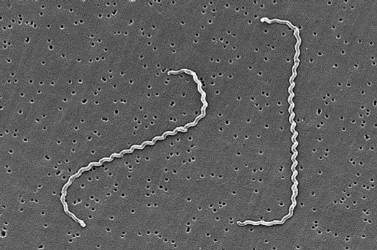
Highly Magnified image of Leptospira spirochetes.
(Photocredit: CDC Public Health Image Library)
|
|
|
From here, Leptospira interrogans sensu lato has been sub-classified into smaller related groups called SEROVARS. Over 250 serovars have been been named and at least 10 are important for pets. Different serovars produce different types of disease and are in different geographical areas. Vaccine for dogs, however, exists against only four serovars.
Canicola - This serovar is the most common in Mexico. It produces primarily kidney disease. With a constant influx of dogs across the border, this is a serovar to watch for in particular.
Pomona - This serovar has an association with livestock and tends produce severe disease in both the kidney and liver.
Grippotyphosa - In a survey of over 1200 healthy dogs in Michigan, 24% of dogs tested as exposed to Leptospira and the Grippotyphosa serovar was the most common.
Icterohaemorrhagiae -This serovar is mostly associated with exposure to rats and rat urine in standing water. Its predilection is for attack on the liver.
|
|
|

A survey in Connecticut found 36% of racoons had been exposed
while a survey in Illinois found 48% of raccoons had been exposed.
Another survey found 50% of rats had been exposed.
(Photocredit: Morguefile.com) |
Leptospires live best in warm, slow-moving water such as after heavy rains or even flooding. After the water clears, they contaminate soil for many months. Wildlife are common carriers of infection. Classically, infection of dogs (and humans) stems from the urine of infected animal getting into environmental water. Leptospirosis is a common human disease in tropical areas especially where rice is farmed and rats infest the paddies. It is believed that rat populations are involved in the rising incidence of canine leptospirosis in urban areas and leptospirosis is no longer considered a rural disease. Leptospires can survive for months in contaminated soil.
This all sounds very outdoorsy but it is important to recall that the 2021 Leptospirosis outbreak in Los Angeles started in boarding facilities where dogs are commonly exposed to the urine of other dogs in play yards and kennel drainage pathways. Anywhere with potential urine contact is a potential home for Leptospira organisms.
|
CANINE INFECTION
Dogs become infected by leptospires when abraded (irritated or cut) skin comes into contact with infected urine or with water contaminated with infected urine. Alternatively, bite wounds, exposure to reproductive secretions, and even consumption of infected tissues can transmit this infection. The organisms quickly spread through the bloodstream leading first to inflammation of the blood vessels themselves: fever, abnormal bleeding, abnormal bruising and tissue edema after an approximately 7 day incubation period. By two weeks post-infection, the leptospires have set up shop in the kidneys where they continue to generate inflammation, pain, and potentially total kidney failure with inability to produce urine. Some serovars also go to the liver and generate inflammation there, though the liver disease is generally not as severe as the kidney disease.
A particularly devastating situation occurs if the organism homes to the lungs where the leptospire toxins produce what is termed "Leptospira Pulmonary Hemorrhage Syndrome." The lung bleeding that results is associated with a 70% mortality rate and bodes especially poorly.
If the dog is able to keep the acute illness at bay, a chronic form may emerge. There can be a more chronic kidney insufficiency and/or hepatitis. Further, the long term immune stimulation can lead to a deep eye inflammation called "uveitis" which can cause the eyes to look cloudy or even change color. If the disease is treated in this form, it may not be possible to reverse the long term damage that has already set in.
THE DIFFERENT CLINICAL PICTURES OF LEPTOSPIROSIS
As one might infer from the above description, Leptospirosis can look very different: fever with bruising, and bleeding, fever with different degrees of kidney failure, liver disease and kidney disease together, chronic hepatitis and eye inflammation etc. Another way to look at Leptospirosis is to look at the time frame of the illness and how quickly or slowly it came on.
PERACUTE DISEASE: Peracute disease means super-sudden onset. These are usually younger dogs with an overwhelming exposure. The large amount of Leptospire toxin causes rapid death before the kidney or liver disease even happens.
ACUTE DISEASE AND SUBACUTE DISEASE: This is more the classic form described above: fever with bruising and bleeding, general muscle pain, painful belly from the kidney and/or liver disease. There may be jaundice and inflammation present in the eyes making them look cloudy.
CHRONIC DISEASE: Recurring fevers, chronic hepatitis, chronic kidney disease, uveitis, poor appetite, weight loss.
YOUNGER DOGS (< 1 YEAR OF AGE) TEND TO GET THE MOST SEVERE FORMS OF LEPTOSPIROSIS.
87-100% OF INFECTED DOGS WILL HAVE SOME DEGREE OF AZOTEMIA
(WHICH MEANS RENAL PARAMETERS WILL BE ELEVATED ON ROUTINE BLOOD TESTING)
Excessive water consumption is frequently observed at home when this happens.
TESTING
PCR Testing
PCR testing is used to detect Leptospire DNA. A blood sample is best in the first 10 days after infection but after that a urine sample is more likely to be positive. It may be prudent to submit both blood and urine samples to be complete. Past vaccination will not interfere with this test (though antibiotic exposure certainly will) and results can be back in a matter of days.
PCR testing will not determine which serovar is present.
MAT Testing (the Traditional Test)
The Microscopic Agglutination Test or MAT test is still considered the test of choice though it has some disadvantages. It measures antibody levels against different Leptospirosis serovars with the idea being that the one with the highest level is most likely to be the serovar causing the disease.
Antibody levels are expressed as titers, which are ratios reflecting how much dilution of the sample is needed before it is too dilute to detect antibodies. For example, a titer of 1:32 means the serum diluted out 32 times still had detectable antibody. A titer of 1:32 may sound pretty high but it is actually pretty low; an MAT titer must be at least 1:800 to be considered positive. If the serovar under consideration is one that might have been included in a past vaccination, the titer must be higher (1:3200) to be considered positive. To really obtain high confidence in the diagnosis of Leptospirosis, a second titer is submitted 2-4 weeks later showing at least a four-fold increase in antibody production. Treatment with antibiotics should not interfere with the validity of the second (or "convalescent") titer level.
There are two problems with this testing:
1) No one wants to wait 2-4 weeks to confirm the diagnosis especially with a disease contagious to humans. PCR testing gets results much faster.
2) Vaccination interferes with results (remember the entire goal of vaccination is to generate an antibody titer). Vaccination history can make interpretation difficult.
In-House Test Kits and Other General Antibody ELISA tests
Recently in-house screening tests have become available so that a screening result can be obtained in 20 minutes or so. These tests screen for antibodies against Leptospira organisms. They are either positive or negative. They will not tell you which serovar is involved and they will not tell you how high the titer is. They will not distinguish antibodies from vaccination versus those from true infection. Clearly a positive test needs to be followed by another test. A negative test, however, is very helpful (see below).
Other Tests
In the past cultures and darkfield microscopy were used to detect leptospires. This technology has largely been consigned to the past.
Which Tests to Use?
A good approach is to begin with a general antibody test combined with urine and blood PCR testing. If any PCR test detects Leptospira DNA either in blood or in urine, infection is confirmed. An MAT test will determine which serovar is afoot and the antibody level can be tracked to be sure treatment is working.
If the PCR tests are negative (meaning Leptospira DNA was not detected) but a general antibody test is positive, the MAT test will determine if the antibodies are related to prior vaccination or active infection.
If PCR tests are negative (Leptospira DNA not found) and no antibodies are found either, then it should be safe to cross leptospirosis off the list of possible diagnoses.
Treatment
Fortunately, Leptospira interrogans sensu lato is sensitive to doxycycline, a readily available antibiotic. Leptospires are cleared from the blood within 24 hours of starting antibiotic treatment but after 48 hours on antibiotics, it is no longer necessary to wear gloves or goggles during handling or clean up. Infected animals should be isolated from other animals at least until their antibiotic course is complete and probably for a couple of weeks after. Check with your veterinarian for instructions.
Intravenous fluids are crucial to support blood flow through the damaged kidneys so that recovery is possible. Any areas at home that have been contaminated with urine should be disinfected with an iodine-based product and gloves should be warn while cleaning up any urine. Prognosis is guarded depending on the extent of organ damage with appropriate treatment 80-90 percent survival rates are reported.
This sounds wonderful but it is important to keep in mind factors that can interfere with this rosy outcome. While most leptospirosis-related kidney injury responds to fluid therapy as can be performed by most animal hospitals, more severe cases can require dialysis which has limited availability. As mentioned, lung involvement has very poor survivability. Infection with the Pomona serovar is associated with more severe disease.
A good two weeks of doxycycline is generally needed. If this antibiotic is not tolerated by the patient, amoxicillin may also work.
PREVENTION
Vaccination against Leptospira interrogans sensu lato is only available for the serovars called Canicola, Grippotyphosa, Pomona and Icterohaemorragiae. (Some vaccines cover all four serovars while others cover only two out of four.) As a result of long standing use of this vaccine, it is hard to assess how important it is to vaccinate against leptospirosis. (As you might imagine, most recent outbreaks involve serovars for which vaccination does not exist,which suggests that the vaccine is working.) Vaccination against Canicola and Icterohaemorragiae has been traditional for dogs as it is included in the basic distemper shot (DHLPP - the “L” stands for leptospirosis). Current guidelines are for all dogs to be vaccinated against Leptospirosis regardless of breed, size, or whether they are urban or rural in lifestyle.
In the past, leptospirosis vaccine was felt to be associated with a higher chance of immunological vaccine reactions, but vaccines made from leptospires grown in protein-free media have made vaccination reaction less likely. Vaccination reactions considered to represent the normal vaccination process include fever, swelling at the injection site, and joint/muscle pain. These symptoms should resolve after a day or so. Small dogs are more likely to experience reactions. Consider pre-treatment with antihistamines prior to vaccination.
Previously infected dogs may become re-infected. Past infection does not confer future immunity.
Other important aspects of prevention include controlling rodents in the pet's environment and removing standing water.
The Infection in Humans
As the Centers for Disease Control and Prevention monitor leptospirosis cases in people, it seems that one third come from contact with infected dogs and one third come from contact with rats (usually through field work). Recreational activities involving water and exposure to flood waters are also associated with human leptospirosis outbreaks. Other human risk factors include farm work, animal care work, camping, and sewer work. Remember, leptospires come from contaminated urine which, in turn, contaminates environmental water and soil.
The same disease symptoms occur in humans as would be seen in dogs.
Links
Leptospirosis in Los Angeles County
Reference laboratories have only been sharing diagnostic results with the Health Dept. since 2014. Since pet owners bear the brunt of testing costs, Leptospirosis is considered to be under-reported. To view local trends, visit:
www.publichealth.lacounty.gov/vet/Leptospirosis2021.htm
(if this link does not connect, copy and paste this URL in a new browser window)
CDC LINK TO HUMAN LEPTOSPIROSIS
https://www.cdc.gov/leptospirosis/

Page last revised: 3/16/2026
|