|
IMMUNE-MEDIATED THROMBOCYTOPENIA

(Immune Destruction of Blood Platelets)
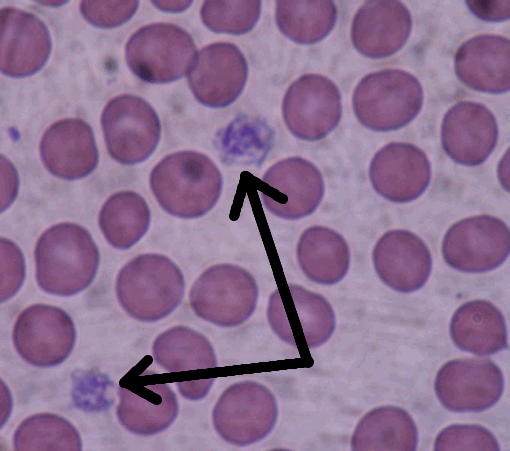
Arrows point to two platelets amid a group of red blood blood cells
(Photo Credit: Bob J. Galindo via Wikimedia Commons)
WHAT IS A PLATELET?
A platelet is a cloud-shaped blood cell, neither related to the red blood cell line nor the white blood cell line. Platelets assist in the clotting of blood in that they home to damaged areas of blood vessels, and “aggregate” there, meaning that they pile onto each other and bind, forming a small plug to seal the hole in the leaking blood vessel. While piled on each other, they release assorted biochemicals initiating a more permanent fibrous seal of the tear. Of course, large tears are too big for platelets to seal but when it comes to small bleeds and normal blood vessel wear and tear, platelets are the star of the show.
There is a saying that “platelets are vascular integrity and vascular integrity is platelets.”
A small bleed unstaunched by a platelet aggregation quickly becomes a large bruise. Spontaneous bruising (in other words visible bruising from the normal wear and tear of one’s body) is a sign of reduced platelet numbers or poor platelet function.
Small abnormal bruises are called "petechiae" or "petechial hemorrhages."
Large abnormal bruises are called "ecchymoses" or "ecchymotic hemorrhages."
THE LIFE AND TIMES OF JOE PLATELET
|
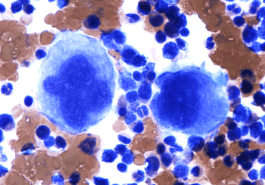
A bone marrow megakaryocyte
(Photocredit: Simon Caulton via Wikimedia Commons)
|
We would like to present a more detailed explanation of a platelet’s life from beginning to end. Platelets come from the bone marrow where a large (actually gigantic relative to the red and white blood cell precursors) cell called a “megakaryocyte” spits off little active pieces of itself. These pieces are platelets, ready to enter the circulation where they will live for an average of 8-12 days (in the dog) or 6-8 days (in a human) before a bleeding capillary calls them to their destiny. At any given time some 200,000-500,000 platelets are on patrol in the circulation, though only about 20,000 to 50,000 are considered the bare minimum to prevent spontaneous bruising and bleeding. About 1/3 of the circulating platelets are actually stored in the spleen, like boats in a harbor, ready to mobilize if necessary. When platelets become too old to be useful, the spleen has special cells called “phagocytes” which essentially eat old cells and recycle their inner materials.
|
IMMUNE-MEDIATED PLATELET DESTRUCTION
For reasons unknown, platelets can be mistaken by the immune system for invaders.. When this happens, antibodies coat the platelets and the spleen’s phagocytes remove them in numbers up to 10 times greater than the normal platelet removal rate. The megakaryocytes in the bone marrow respond by getting larger and growing in numbers so that they may increase their production of platelets. The platelets produced under these circumstances tend to be larger and more effective than normal platelets and are called “stress platelets.” The bone marrow attempts to overcome the accelerated platelet destruction rate; unfortunately, with immune-mediated destruction occuring, a human platelet can expect to survive only one day in the circulation instead of its normal 6-8 days. If antibody levels are very high, a platelet may survive only minutes or hours after its release from the bone marrow and, making matters worse, antibody coated platelets still circulating do not function normally. This is balanced by the especially effective stress platelets entering the scene so that overall it is hard to predict how the balance will work out in a given patient.
WHAT WOULD CAUSE THE IMMUNE SYSTEM TO GET SO CONFUSED?
In many cases, a cause is never found; however, in cases a primary reaction in the immune system precedes the platelet destruction. Keep in mind that the immune system responds to the shapes of proteins present on a cell’s surface. These shapes are similar to ID cards. The immune system recognizes shapes defined as “self” and does not attack but when it sees a cell expressing protein shapes that are “non-self,” it will respond.
If the immune system is responding to a blood parasite, tumor, drug, or other cell type (as in lupus or immune-mediated red cell destruction), it will be producing antibodies against “enemy” shapes. Some of these shapes may, unfortunately, resemble some “self” shapes such as some of the shapes on the surface of the platelets. The platelets are then mis-identified as the enemy and are attacked. Alternatively, foreign proteins may actually stick to the platelet surface thus fooling the immune system to respond to the platelet as a whole.
|
WHAT HAPPENS TO THE PATIENT?
The usual patient is a middle-aged dog. Poodles appear to be predisposed though Cocker Spaniels and Old English Sheepdogs also seem to have a higher than average incidence of this condition.
Spontaneous bruising is the major clinical sign. The gums and oral surfaces as well as the whites of the eyes are obvious areas to check as is the hairless area of the belly. Small spots of bruising in large conglomerations called “petechiae” (“pet-TEEK-ee-a”) are the hallmark sign. A large, purple expansive bruise might also be seen. This is called “ecchymosis.” Large internal bleeds are not typical of platelet dysfunction, though bleeding small amounts in urine, from the nose, or rectally may also indicate a platelet problem.
When these sorts of signs are seen, a platelet count is drawn, along with usually an array of clotting parameters, red blood cell counts to assess blood loss, and other general metabolic blood tests. Since testing to detect actual anti-platelet antibodies is not available, the veterinarian must determine if any other possible causes of low platelet count make sense.
|



(Photocredit: Morguefile.com)
|
OTHER CAUSES OF PLATELET DYSFUNCTION
|
Dramatic reduction in platelet numbers is almost always caused by immune-mediated destruction, though certain tick-borne blood parasites could also be responsible (or could be the initiators of the immune response):
- Ehrlichiosis (especially infection with Ehrlichia platys which has recently been renamed Anaplasma platys)
- Neorickettsia rickettsii (Rocky Mountain Spotted Fever)
If an infectious agent such as one of these is responsible for the immune-mediated platelet destruction, obviously specific therapy against the infection is warranted in addition to therapy for the platelet destruction.
Very low platelet counts can also occur in response to the suppression of megakaryocytes within the bone marrow. This might be caused by:
|
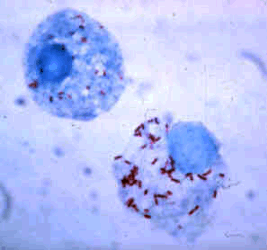 Neorickettsia rickettsia organisms (staining red) inside host blood cells. Neorickettsia rickettsia organisms (staining red) inside host blood cells.
(Photocredit: CDC Public Domain Image) |
Disseminated Intravascular Coagulation is a life-threatening disastrous uncoupling of normal blood clotting and clot dissolving functions in the body and one of its hallmark signs is a drop in platelet count (along with a constellation of other signs).
If platelet numbers are normal but it is obvious that platelet function is not, some other causes to look into might include:
THERAPY FOR IMMUNE MEDIATED PLATELET DESTRUCTION
Once a tentative diagnosis of immune-mediated platelet destruction has been made, the goal in therapy is to stop the phagocytes of the spleen from removing the antibody-coated platelets by cutting off antibody production. This, of course, means suppression of the immune system using whatever combination of medication seems to work best for the individual patient.
Prednisone or Dexamethasone
These steroid hormones are the first line of defense and, often, all that is necessary in bringing platelet counts back up. Unfortunately, long term use should be expected and this means steroid side effects are eventually inevitable: excessive thirst, possible urinary tract infection, panting, poor hair coat etc. The good news is that these effects should resolve once medication is discontinued; further, if side effects are especially problematic, other medications can be brought in to reduce the dose of steroid needed.
Vincristine
This injectable medication is mildly immune suppressive but also seems to stimulate a sudden burst of platelet release from the marrow megakaryocytes. The platelets released in response to vincristine contain a phagocyte toxin so that when they are ultimately eaten by spleen phagocytes, the phagocytes will die. While repeated injections of vincristine ultimately do not yield the same effect, at least a one time dose may be extremely helpful. One should note that vincristine is extremely irritating if delivered outside of the vein. It must be given IV cleanly or the overlying tissue will slough.
Androgens
Male hormones may have some masculinizing side effects but they do seem to cut production of anti-platelet antibodies. It also seems to synergize with the corticosteroid hormones like prednisone and dexamethasone. Danazol has been the androgen typically recommended in the treatment of immune-mediated platelet destruction with weight gain being the most common side effect.
Azathioprine or Cyclophosphamide
These are stronger immune suppressive agents typically used in cancer chemotherapy. If steroid side effects are unacceptable or if the patient does not respond to steroids alone, one of these medications may be indicated. Cyclosporine, a newer medication made popular in organ transplantation, also may be used but expense has been problematic.
|
TRANSFUSION
One might think that a transfusion of blood or at least “platelet rich plasma” might be helpful in the treatment of a platelet dysfunction. The problem is that platelets do not survive well after removal from a blood donor. One has about 12 hours to deliver the freshly withdrawn blood to the recipient before the platelets become inactive. After the platelets are delivered they are likely to live only hours. In general, most efforts are spent on establishing immune suppression.
GAMMA GLOBULIN TRANSFUSION
Gamma globulins are blood proteins including antibodies. Human gamma globulin appears to occupy the phagocyte antibody binding site so that coated platelets cannot be grabbed out of the circulation. This has been a promising therapy for both humans and dogs but is generally prohibitively expensive.
|
(original graphic by marvistavet.com)
|
SPLENECTOMY
(original graphic by marvistavet.com)
If medication simply does not work or the condition keeps recurring once medications are discontinued, the solution may be to simply remove the spleen. After all, this is where the phagocytes removing the platelets are primarily located. In humans, immune-mediated platelet destruction is generally treated with splenectomy first. Response in dogs has not been as predictably good thus in veterinary medicine it is generally one of the last therapies invoked.

Page last updated: 6/16/2017
|