|
NORMAL JOINT STRUCTURE

A pet does not have to be a senior citizen to require joint care supplements, pain medication, or physical therapy. Degenerative arthritis can result from an injury or can be the result of genetics/joint conformation. If your pet is having stiffness, or poor range of motion in a joint then you will need some education about joint care options and an understanding of what is happening in your pet's joints, especially if surgery is not feasible for one reason or another. The following represents a beginner's overview of joint structure and function so as to provide a foundation for understanding treatment options for the arthritic pet.
|

The canine knee joint:
a common site for arthritis.
(original graphic by marvistavet.com)
|
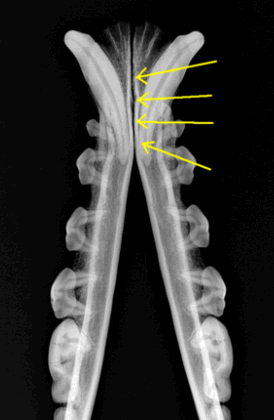
This radiograph shows the two
mandibles (lower jaw bones) of a dog.
The yellow arrows point to the
"symphysis" joint which joins them
(original graphic by marvistavet.com)
|
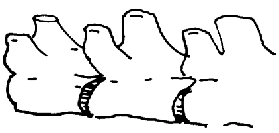
The vertebral bones are joined together
by round disc joints which allow
the back to have flexibility
(original graphic by marvistavet.com)
|
THE STRUCTURE OF A NORMAL JOINT
|
There are several types of joints within the body. The fibrous disks that separate the back’s vertebrae and allow the back’s flexibility are specialized joints (shown in the illustration above.) The two halves of one’s lower jaw are held together by a joint called a “symphysis” which, unlike other joints, is meant to reduce movement, not facilitate it (also above.)
The joints we are concerned with when we talk about degenerative arthritis are the “synovial joints” also called “diarthrodial joints." They consist of two bones and a fibrous capsule holding the two bones together; however, the joint is far more complicated than just a hinge made of fiber and bone. The two bones have surfaces that are covered with slippery cartilage that must be able to glide across each other with minimal friction no matter what the patient’s activity level is and they must continue to be able to glide easily in this way repeatedly throughout the patient’s life. Further, the joint capsule secretes assorted nutrients, lubricating fluid, and immunological materials keeping the joints healthy.
Prevention of the progression of arthritis is all about maintaining the normal structures of the joint. In many cases, this involves providing the biochemical components of these structures as nutritional supplements. Our purpose here is to review what the structures are and what they are made of so that one can better choose supplements and understand what one is giving. For illustrative purposes we will use the shoulder joint as an example. The illustration at the right shows the structures of the shoulder.
|
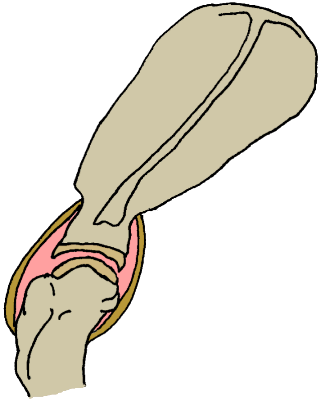
The shoulder joint involves the scapula (or shoulder blade)
and the head of the humerus (arm bone). The bone
surfaces are lined with cartilage and the entire joint
is encased in a fibrous capsule called a joint capsule.
(original graphic by marvistavet.com)
|
ARTICULAR CARTILAGE SURFACES
|
The articular cartilage surfaces of the joint are the cartilage caps on the ends of the bones. These are the smooth surfaces that must glide across each other with minimal friction. Any rough spots will ultimately abrade over time and create pain and inflammation.
Cartilage is made up of cartilage cells called "chondrocytes" and the special "matrix" in which they live (think of fruit chunks suspended in a "matrix" of jello). The matrix is made of the all-purpose structural protein called "collagen" (probably a familiar word) and "proteoglycan" (probably an unfamiliar word). The matrix is made to retain water like a sponge thus creating a soft “shock absorber” for the joint.
MORE ABOUT WHAT’S IN THE MATRIX
(because you are probably feeding it to your pet if you use a joint supplement)
So we’ve already said the matrix consists of collagen (steel girders for your body’s structure) and proteoglycan (the spongy stuff). When we give “chondroprotectants” or “cartilage building blocks” as supplements we are basically providing the materials that make up proteoglycan so that the body will have plenty of ingredients to make fresh cartilage matrix.
Here is a depiction of a piece of proteoglycan:
|
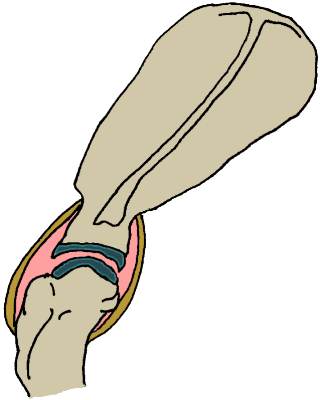
Same depiction of the shoulder joint.
The articular cartilages are shown in grey-blue.
(original graphic by marvistavet.com)
|
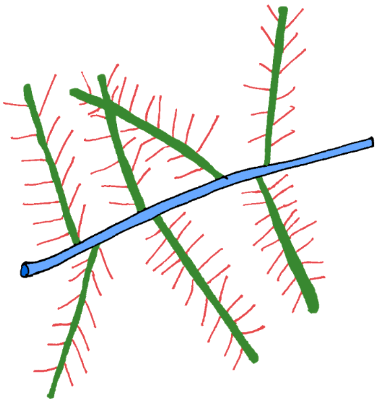
Proteoglycan depiction: core proteins in green, GAG "bristles" in red, hyaluronic acid in blue.
(original graphic by marvistavet.com)
The core proteins (shown in green) have bottlebrush like GAG (glycosaminoglycan) molecules coming off them ready to soak up water. These GAGs include keratan sulfate (made from glucosamine), and chondroitin sulfate, both being very common oral joint supplements. Connecting these GAGs together are big molecules of hyaluronan (also called "hyaluronic acid"). Hyaluronan is another GAG that helps make for a good water-rich cartilage by networking the other molecules together plus it is secreted by the joint capsule and is an important component of the actual lubricating joint fluid.
The point is that you are probably going to be including a glucosamine and/or chondroitin sulfate supplement in your pet’s regimen and now you know what it is for: replenishing the cartilage matrix so that it can properly soak up water and be an effective shock absorber. You may also be considering hyaluronan joint injections to improve joint lubrication. Now you have a better understanding of how these treatments work.
|
THE JOINT CAPSULE OR “SYNOVIAL MEMBRANE”
This is the capsule that encloses the joint, creating the structure of the “hinge.” The capsule has an outer tough, fibrous layer and an inner layer that secretes joint fluid, a fluid that provides both nutrition and lubrication to the enclosed joint. The joint capsule must keep unwanted proteins and biochemicals out of the joint and only let the desired nutrients inside. After all, the joint must be kept smooth, and the lubricants pure if they are to maintain the joint throughout the patient’s entire lifetime.
The joint capsule has two types of cells: Type A Synoviocytes and Type B Synoviocytes. The Type A cells are all about removing impurities and cleaning up debris. Type B cells produce Hyaluronan (mentioned above), an important lubricant in the joint.
|
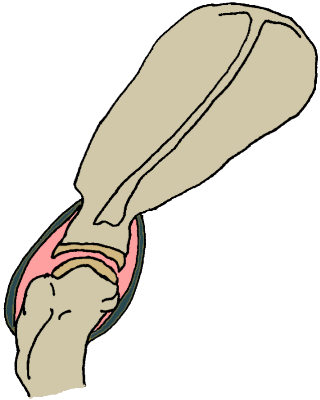
Same depiction of the shoulder joint.
The joint capsule is shown in dark green.
(original graphic by marvistavet.com)
|
When there is injury or simply poor conformation, the cartilage becomes roughened and can chip, flake off, or even wear down. The joint capsule becomes inflamed and thickened and no longer functions normally. Impurities enter the joint, the lubricating fluid loses its natural properties and ultimately a progressively abnormal and painful joint is created. In providing treatment, our goal is to alleviate the pain and inflammation and provide the biochemical building blocks that allow the joint to heal itself. In the next sections we will review medications, supplements, and even exercises that may help with the arthritic patient.
[Back to Arthritis/Joint Disease Information Center]

Page last updated: 6/22/2025
|