|
CANINE PANCREATITIS

|
THE NORMAL PANCREAS AND WHAT IT DOES
We eat food, chew it up into a slurry, and swallow it. It travels down the esophagus to the stomach where it is ground up further and enzymes are added to begin the break-down of dietary nutrients (“digestion”). When the food particles are small enough, they are propelled into the small intestine for further digestive treatment and ultimately nutrient absorption. The upper part of the small intestine (the duodenum) is for further digestion/break down of nutrients while the lower parts of the small intestine are for absorption of the digested nutrients.
The pancreas is a pale pink glandular organ that nestles cozily just under the stomach and along the duodenum. As a glandular organ, the pancreas is all about secretion and it has two main jobs: the first job is the secretion of digestive enzymes to help us break down the nutrients we eat, the second job is the secretion of insulin and glucagon (to regulate how we use the nutrients we eat). It's the first job (the digestive enzyme part) that concerns us in pancreatitis.
|
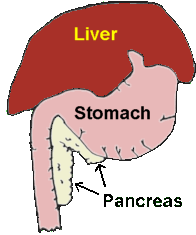
(original graphic by marvistavet.com)
|
|
PANCREATITIS IS INFLAMMATION OF THE PANCREAS
In pancreatitis, inflammation disrupts the normal integrity of the pancreas. Digestive enzymes are normally stored safely as inactive forms within pancreatic granules so that they are harmless. In pancreatitis they are prematurely activated and released internally, digesting the body itself. The result can be a metabolic catastrophe. The living tissue becomes further inflamed and the tissue damage quickly involves the adjacent liver. Toxins released from this rampage of tissue destruction are liberated into the circulation and can cause a body-wide inflammatory response. If the pancreas is affected so as to disrupt its ability to produce insulin, diabetes mellitus can result; this can be either temporary or permanent.
SPECIAL PANCREATITIS DISASTERS
|
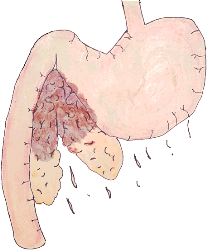
Swollen, inflamed pancreas with areas of hemorrhage
(original graphic by marvistavet.com)
|
- Special disasters include the disruption of “surfactants” in the lung tissue which normally keep the tiny air-filled alveoli from collapsing after each exhaled breath. Without surfactants, the alveoli close up and respiratory failure results.
- Also, there is a special syndrome called “Weber-Christian syndrome” where fats throughout the body are destroyed with painful and disastrous results.
- Pancreatitis is one of the chief risk factors for the development of what is called “disseminated intravascular coagulation” or “DIC” which is basically a massive uncoupling of normal blood clotting and clot dissolving mechanisms. This leads to abnormal simultaneous bleeding and clotting of blood throughout the body.
- Pancreatic encephalopathy (brain damage) can occur if the fats protecting the central nervous system become digested.
The good news is that most commonly, the inflammation
is confined to the area of the liver and pancreas
but even with this limitation, pancreatitis can be painful and life-threatening.
Pancreatitis can be acute or chronic, mild or severe.
WHAT CAUSES PANCREATITIS
In most cases we never find out but we do know some events which can cause pancreatitis:
- Backwash (reflux) of duodenal contents up into the pancreatic duct. The pancreas has numerous safety mechanisms to prevent self-digestion. One of these mechanisms is the fact that the enzymes it creates are stored in an inactive form. They are harmless until they are mixed with activating enzymes. The strongest activating enzymes are made by duodenal cells which means that the digestive enzymes do not actually activate until they are out of the pancreas and mixing with food in the duodenum. If duodenal fluids backwash up the pancreatic duct and into the pancreas, enzymes are prematurely activated and pancreatitis resuls. This is apparently the most common pancreatitis mechanism in humans, though it is not very common in veterinary patients.
- Concurrent hormonal imbalance predisposes a dog to pancreatitis. Such conditions include: Diabetes mellitus, Hypothyroidism, and Hypercalcemia. The first two conditions are associated with altered fat metabolism which predisposes to pancreatitis and the latter condition involves elevated blood calcium which activates stored digestive enzymes.
- Use of certain drugs can predispose to pancreatitis (sulfa containing antibiotics such as trimethoprim sulfa, chemotherapy agents such as azathioprine or L-asparaginase, and the anti-seizure medication potassium bromide). Exposure to organophosphate insecticides has also been implicated as a cause of pancreatitis. Exposure to steroid hormones have traditionally been thought to be involved as a potential cause of pancreatitis but this appears not to be true.
- Trauma to the pancreas as from a car accident or even surgical manipulation can cause inflammation and thus pancreatitis.
- The presence of a tumor in the pancreas can lead to inflammation in the adjacent pancreatic tissue.
- A sudden high fat meal is the classic cause of canine pancreatitis. The sudden stimulation to release enzymes to digest fat seems to be involved.
- Obesity has been found to be a risk factor because of the altered fat metabolism that goes along with it.

(Photo Credit: Public Domain Pictures.net)
Miniature Schnauzers are predisposed to pancreatitis
as they commonly have altered fat metabolism.
SIGNS OF PANCREATITIS
The classical signs in the dog are appetite loss, vomiting, diarrhea, painful abdomen, and fever or any combination thereof.
MAKING THE DIAGNOSIS
|
Lipase and Amylase Levels (no longer considered reliable)
A reliable blood test has been lacking for this disease until recently. Traditionally, blood levels of amylase and lipase (two pancreatic digestive enzymes) have been used. When their levels are especially high, this has been felt to be a reasonable sign that these enzymes have leaked out of the pancreas and pancreatitis is present but, still, these tests are not as sensitive or specific as we would prefer. Amylase and lipase can elevate dramatically with corticosteroid use, with intestinal perforation, kidney disease, or even dehydration. Some experts advocate measuring lipase and amylase on fluid from the belly rather than on blood but this has not been fully investigated and is somewhat invasive.
Pancreatic Lipase Immunoreactivity
A newer test called the “PLI” or “pancreatic lipase immunoreactivity” test has come to be important. As mentioned, lipase is one of the pancreatic digestive enzymes and only small traces are normally present in the circulation. These levels jump dramatically in pancreatitis which allows for the diagnosis to be confirmed with a non-invasive and relatively inexpensive test. The PLI test is different from the regular lipase level because the PLI test measures only lipase of pancreatic origin and thus is more specific. The problem is that technology needed to run this test is unique and the test can only been run in certain facilities on certain days. Results are not necessarily available rapidly enough to help a very sick patient.
|
 (Photocredit: National Institute of Mental Health, National (Photocredit: National Institute of Mental Health, National
Institutes of Health, Department of Health and Human Services) |
Spec CPL and DGGR Lipase Assay
More recently a new test called the SPEC cPL (“specific canine pancreatic lipase”) test has become available. This test is a newer generation immunological test for canine pancreatic lipase and can be run overnight by a reference lab. This test is able to detect 83% of pancreatitis cases (the test is 83% sensitive) and excludes other possible diseases in 98% of cases (i.e. the test is 98% specific for pancreatitis). The CPL test has been adapted into an in-house test kit and can be run in approximately 30 minutes. Some kits provide an actual numeric value while others are simply positive or negative depending on whether the CPL level surpasses the normal level. These kits have made diagnosis of pancreatitis much more rapid and convenient.
A similar lipase assay called the DGGR Lipase Assay (Precision PSL® test). This test can be run at a reference laboratory with results obtained usually overnight; there is no in-hospital test kit.
The diagnosis of pancreatitis is not made solely on the basis of a lab test. It is important to realize that these tests are not used to screen patients that are not sick; the entire clinical picture of a given patient is considered in making this or any other diagnosis.
Imaging
Radiographs can show a widening of the angle of the duodenum against the stomach which indicates a swelling of the pancreas. Most veterinary hospitals have the ability to take radiographs but this type of imaging is not very sensitive in detecting pancreatitis and only is able to find 24% of cases.
|
Ultrasound, on the other hand, detected 68% of cases and provides the opportunity to image other organs and even collect fluid from the belly easily. Since pancreatitis can be accompanied by a tumor in the vicinity of the pancreas, ultrasound provide the opportunity to catch complicating factors such as this.
In some cases, surgical exploration is the only way to make the correct diagnosis.
|
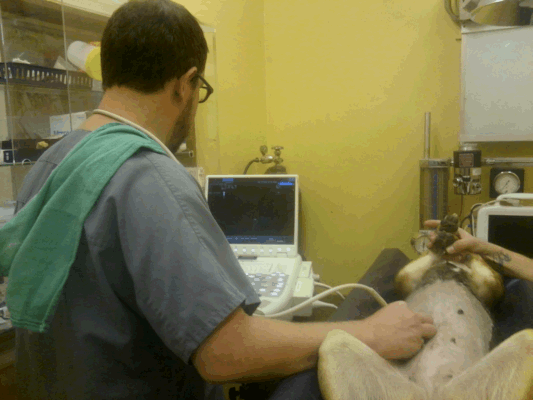
Dr. Jon Perlis of DVMSound at our hospital
performing ultrasound exam.
(original graphic by marvistavet.com)
|
TREATMENT
|
The most important feature of treatment is aggressively rehydrating the patient with intravenous fluids as this restores the circulation to the pancreas and supports the natural healing mechanisms of the body. This means that the best route to recovery involves hospitalization. Fluids are continued until the patient is able to reliably drink and hold down adequate fluid intake, a process which commonly takes the better part of a week. Pain medication and nausea medication are needed to keep the patient comfortable, restore interest in food, and prevent further dehydration.
Plasma transfusion is somewhat controversial in the treatment of pancreatitis. On one hand, plasma replenishes some of the natural blood proteins that are consumed by circulating digestive enzymes and would seem to make sense in pancreatitis treatment. In humans with pancreatitis, however, no benefit has been shown with plasma transfusion. Whether or not the protection afforded by plasma is real or theoretical is still being worked out. Higher mortality has been associated with patients receiving plasma but this may be because they were sicker than patients who did not receive plasma to begin with.
In the past, nutritional support was delayed in pancreatitis patients as it was felt that stimulating the pancreas to secrete enzymes would encourage the on-going inflammation but this theory has been re-thought. Currently, earlier return to feeding has been found to be beneficial to the GI tract's ability to resume function. If nausea control via medication does not produce a reasonable appetite in the patient, assisted-feeding is started using a fat-restricted diet. Return of food interest and resolution of vomiting/diarrhea generally means the patient is ready for return to the home setting. Low fat diets are crucial to management of pancreatitis and their use should be continued for several weeks before attempting return to regular dog food. Some dogs can never return to regular dog food and require prescription low fat foods indefinitely.
Supportive care includes more than just intravenous fluids. Nausea medication, pain relief, and possibly protection of the stomach from ulceration are all commonly included in the treatment plan for a pancreatitis patient. The specifics will be individually tailored for each situation.
HOW MUCH FAT IS OKAY?
There are several ultra-low fat diets made for pancreatitis patients and your veterinarian will likely be sending your dog home with one of them. Remember that pancreatitis is a diet-sensitive disease so it is important not to feed unsanctioned foods or you risk a recurrence. If your dog will not eat one of the commercial therapeutic diets, you will either need to home cook or find another diet that is appropriately low in fat (less than 7 percent fat on a dry matter basis). In order to determine the fat content of a pet food, some calculation is needed to take into consideration how much moisture is in the food.
The Guaranteed Analysis on the bag or can of food will have two values that we are interested in: the % moisture and the maximum % crude fat. (Low fat diets are required to print both a minimum % fat as well as a maximum). To determine the % fat in the food on a dry matter basis, you must first determine the % dry matter of the food. This is done by subtracting the moisture content from 100. For example, if the moisture content is 15%, the dry matter is 85%. If the moisture content is 75%, the dry matter is 25% and so on.
Next, take the maximum % crude fat from the label and divide the % crude fat by the % dry matter. For example, if the moisture content is 76%, this means the dry matter is 24%. If the maximum crude fat content is 4%, the true fat content is 4 divided by 24 which =0.16 (16%). Such a food would be way too high in fat for a dog with pancreatitis. You want the number to be 0.07 (7%) or less. Simply reading the fat content off the label does not take into account the moisture content of the food and will not tell you what you need to know. If this is too much math, the staff at your vet's hospital can help you out.
Of course, if the food is not labelled as a "low fat" diet, it will only have a minimum fat % on the Guaranteed Analysis and the chances are slim that it will be appropriate. The same calculation can be done and if the minimum fat works out to be too high then the maximum fat content will certainly be too high. If the minimum fat content ends up being acceptable, there will be no way to know what the maximum amount is unless the label reports it.
When in doubt, canned chicken, fat-free cottage cheese and/or boiled white rice will work in a pinch.
Eventually, there will be a point where the tests will be repeated and it will be determined if the patient has chronic pancreatitis and will need long term dietary modification or if the episode has concluded. The safest diet going forward will be the prescription low fat diets used during the acute episode but if one wants to transition to a conventional diet this can be done. If one restarts a regular diet, it is prudent to recheck pancreatitis testing in a few weeks to be sure that there is no recurrence on the horizon. Alternatively, a diet can be used with a moderate fat restriction (15% by dry matter as calculated above) might make for a happy medium.
|
|
(original graphic by marvistavet.com)
BEWARE OF DIABETES MELLITUS
When the inflammation subsides in the pancreas, some scarring is inevitable. When 80% of the pancreas is damaged to an extent that insulin cannot be produced, diabetes mellitus results. This may or may not be permanent depending on the capacity for the pancreas’ tissue to recover. For more information on the management of diabetes, see the Diabetes Center on this web site.


Past last updated: 6/29/2021
|